Wart Common (ICD-10: B07) ⚠️
Common Wart (Verruca Vulgaris): Benign Viral Skin Neoplasm
Overview
Common warts, or verruca vulgaris, are benign skin growths caused by infection with the human papillomavirus (HPV), particularly low-risk strains. These warts appear as raised, rough-surfaced lesions that most commonly develop on the hands and fingers. Though they are non-cancerous and generally painless, their visible appearance, tendency to spread, and resistance to treatment—especially in adults—make them a common dermatological concern.
Viral warts are especially prevalent among children and adolescents, affecting nearly 10% of this population. While spontaneous regression is possible (occurring in up to 40% of adolescents), the likelihood of spontaneous resolution decreases with age. Warts are typically multiples, may recur, and frequently prove resistant to conservative therapy—especially in immunocompromised individuals.
Predisposing Factors and Transmission
Warts are caused by specific strains of HPV, which infect the skin through micro-abrasions or damaged epithelial surfaces. While HPV is extremely widespread, not everyone who comes into contact with the virus will develop warts—suggesting a significant role of host immune factors.
Common risk factors for developing verruca vulgaris include:
- Immunosuppression: HIV infection, cancer treatment, or immunosuppressive drugs can facilitate wart development and persistence;
- Metabolic disorders: Diabetes mellitus, obesity, and hormonal imbalances;
- Skin trauma: Chronic friction, scratching, or skin breakdown may facilitate viral entry;
- Poor hygiene: Increases the likelihood of viral transmission in shared spaces (e.g., gyms, pools);
- Pregnancy: Hormonal shifts and immunological changes may increase susceptibility;
- Psychological stress and fatigue: Known to compromise immune surveillance, increasing viral activity;
- Existing chronic skin diseases: Such as eczema or psoriasis may create portals of viral entry.
HPV transmission occurs through direct skin contact with infected tissue or indirectly via fomites—contaminated surfaces, personal items, or tools. Autoinoculation is also possible when individuals touch or scratch one lesion and spread the virus to adjacent skin.
Diagnosis of Common Warts
Diagnosis is typically clinical and based on the lesion’s characteristic appearance. In straightforward cases, no laboratory testing is required. However, diagnostic tools can assist in atypical or persistent cases, especially if malignancy is suspected.
Diagnostic techniques include:
- Visual examination: Identification of classic morphological features such as rough surface, papillary texture, and interruption of normal skin lines;
- Dermatoscopy: Enhances visualization of key internal vascular and structural features of the wart (see below);
- HPV DNA typing: Performed in select cases, especially for genital or resistant warts;
- Biopsy: Indicated in lesions that are rapidly growing, atypical in appearance, or unresponsive to treatment. Histopathology reveals hyperkeratosis, papillomatosis, and koilocytosis.
Clinical Presentation and Symptoms
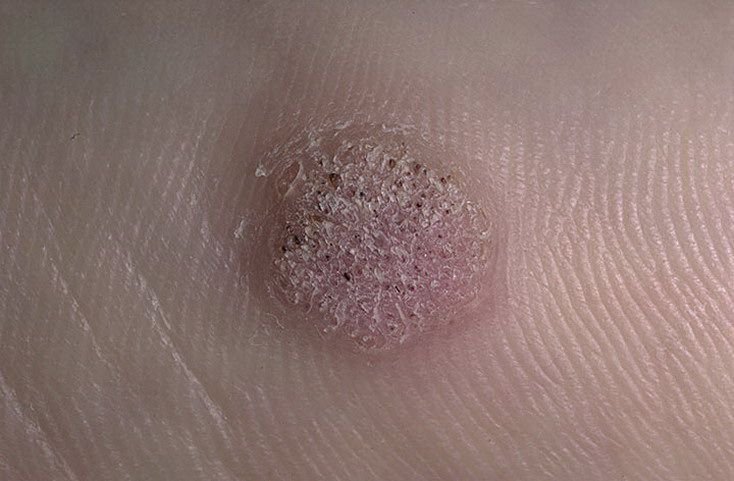
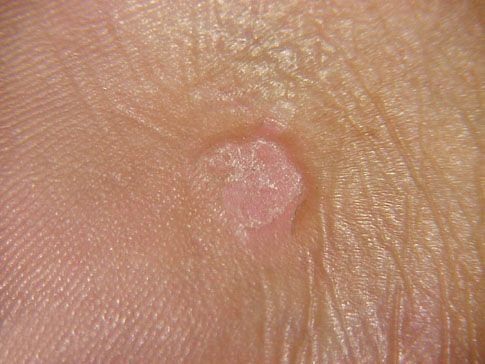
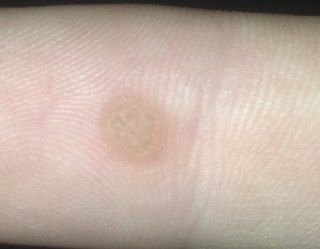
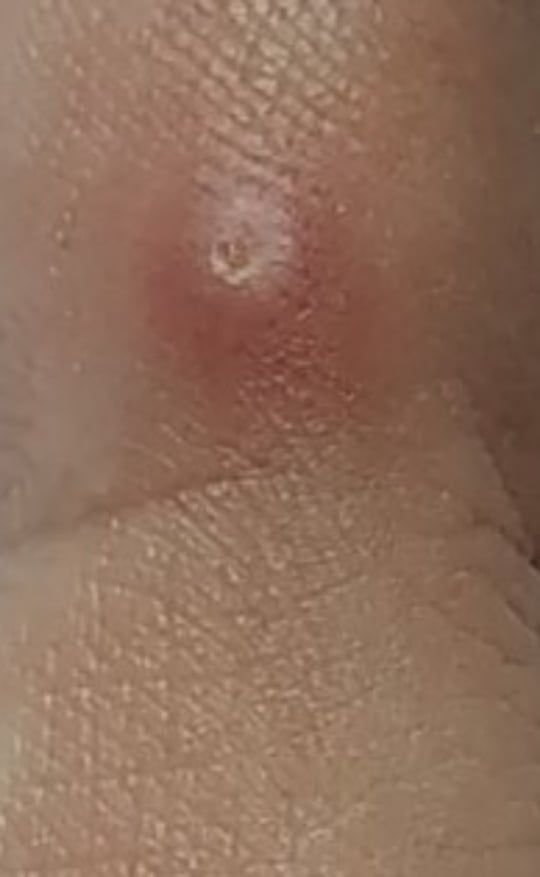
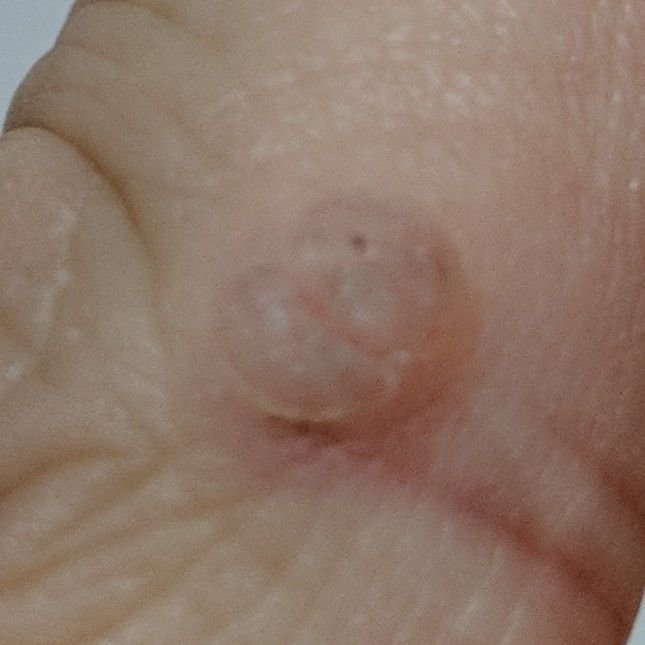
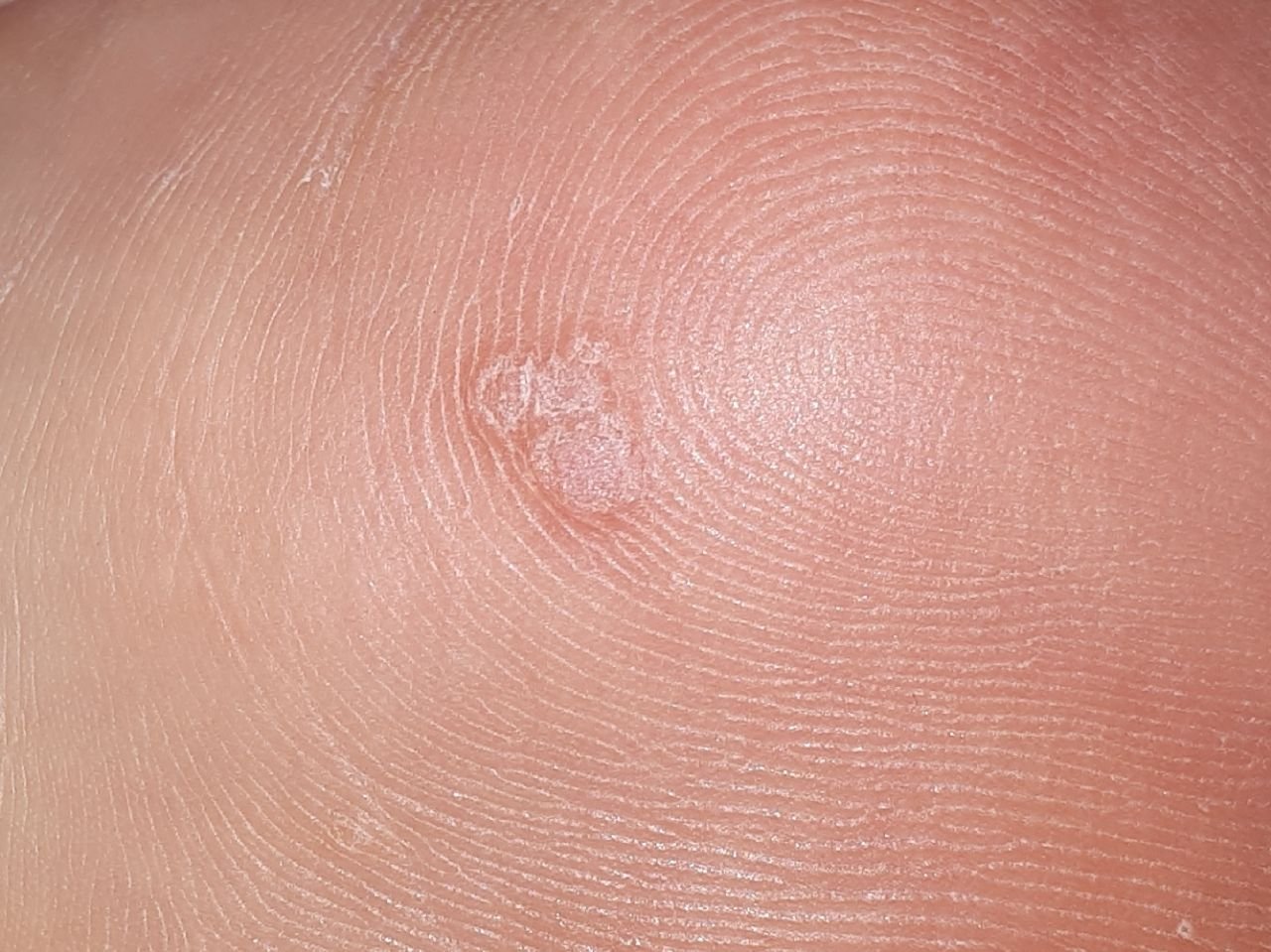
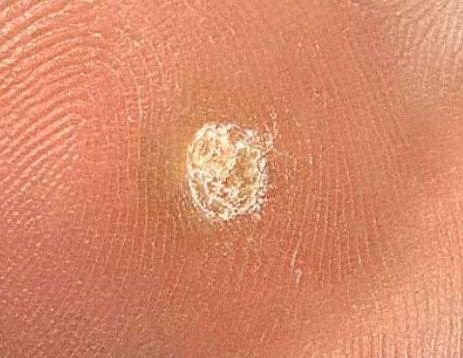
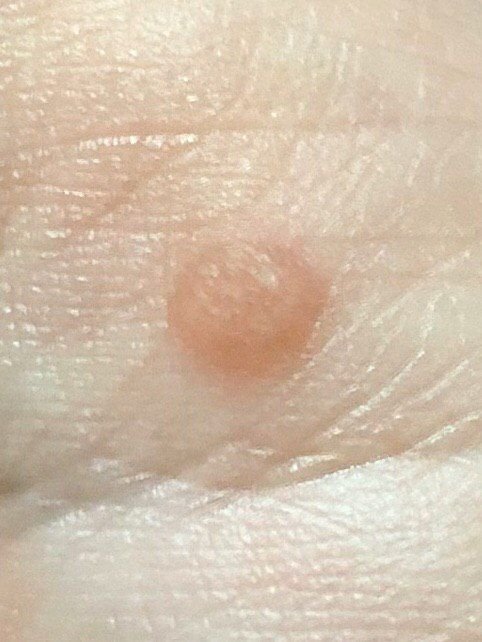
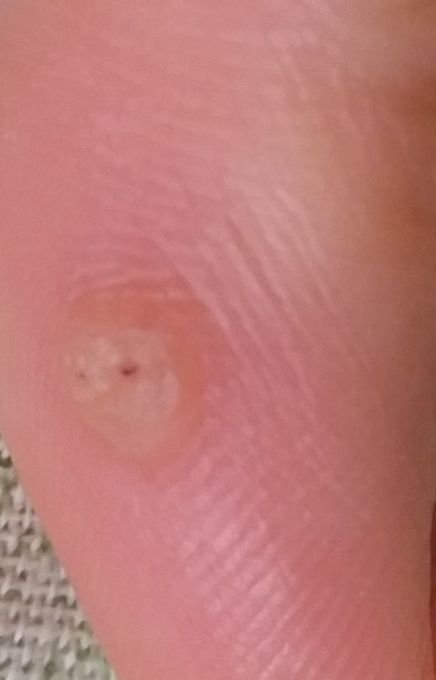
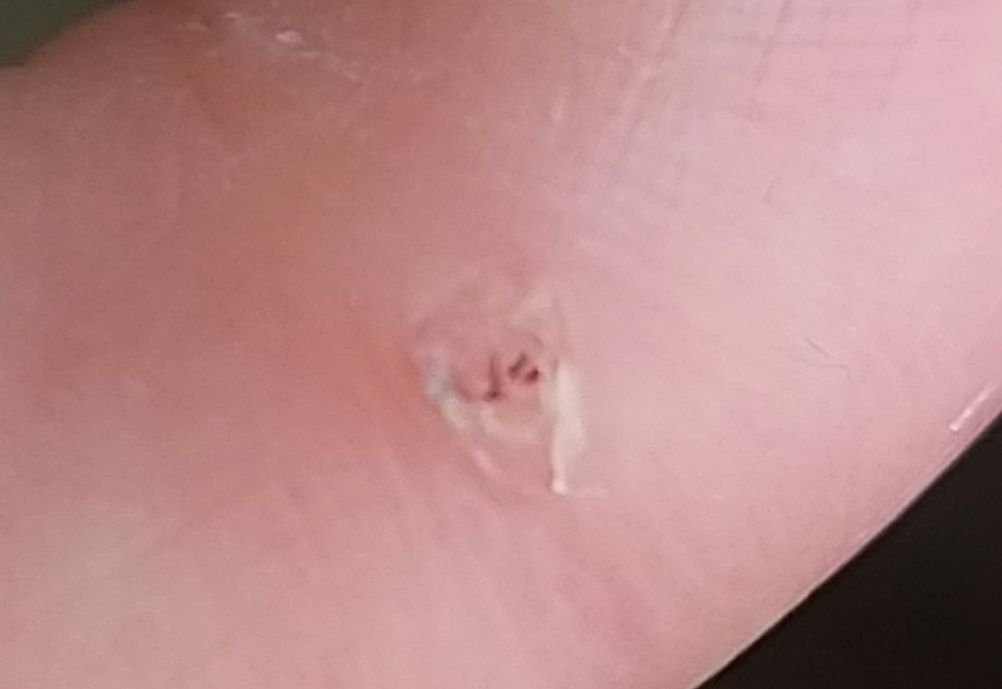
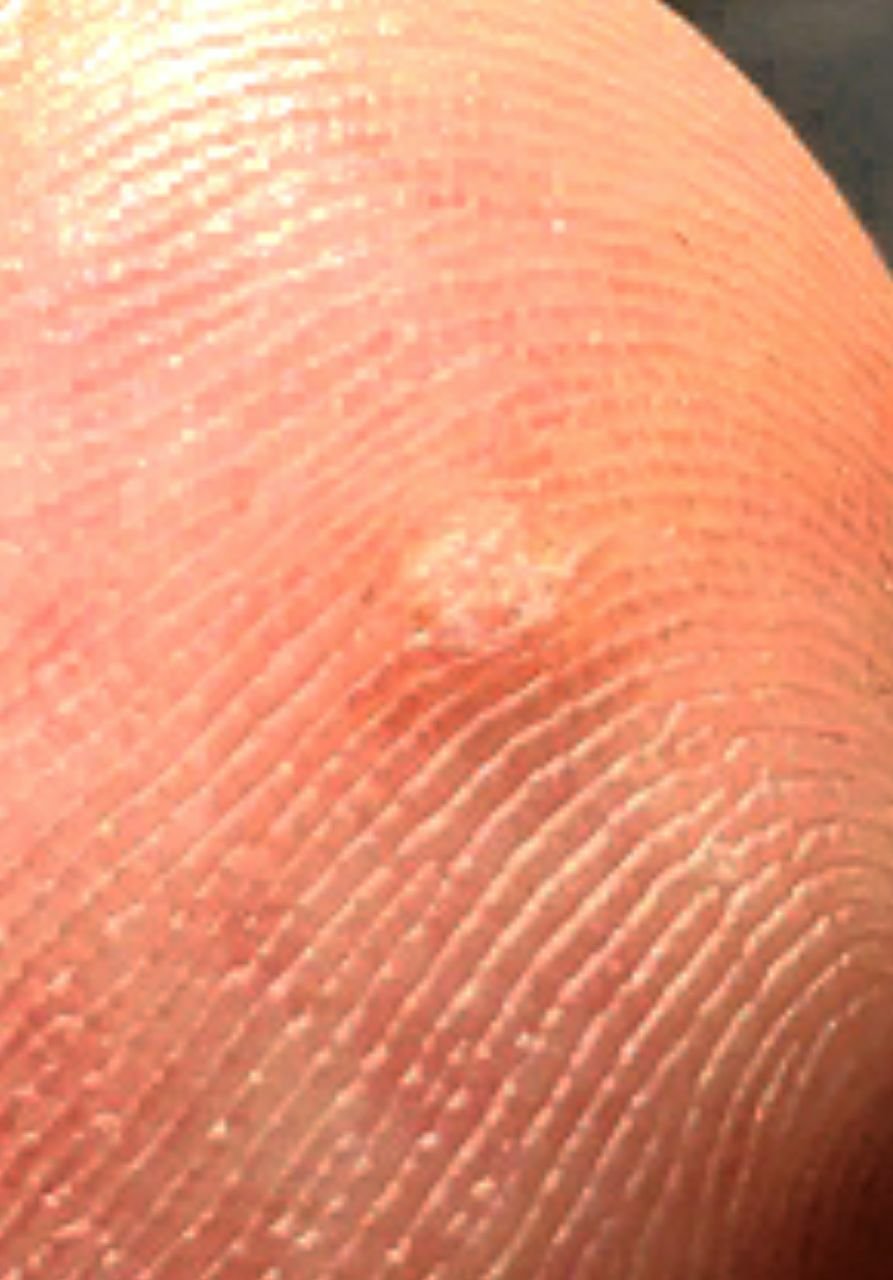
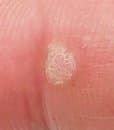
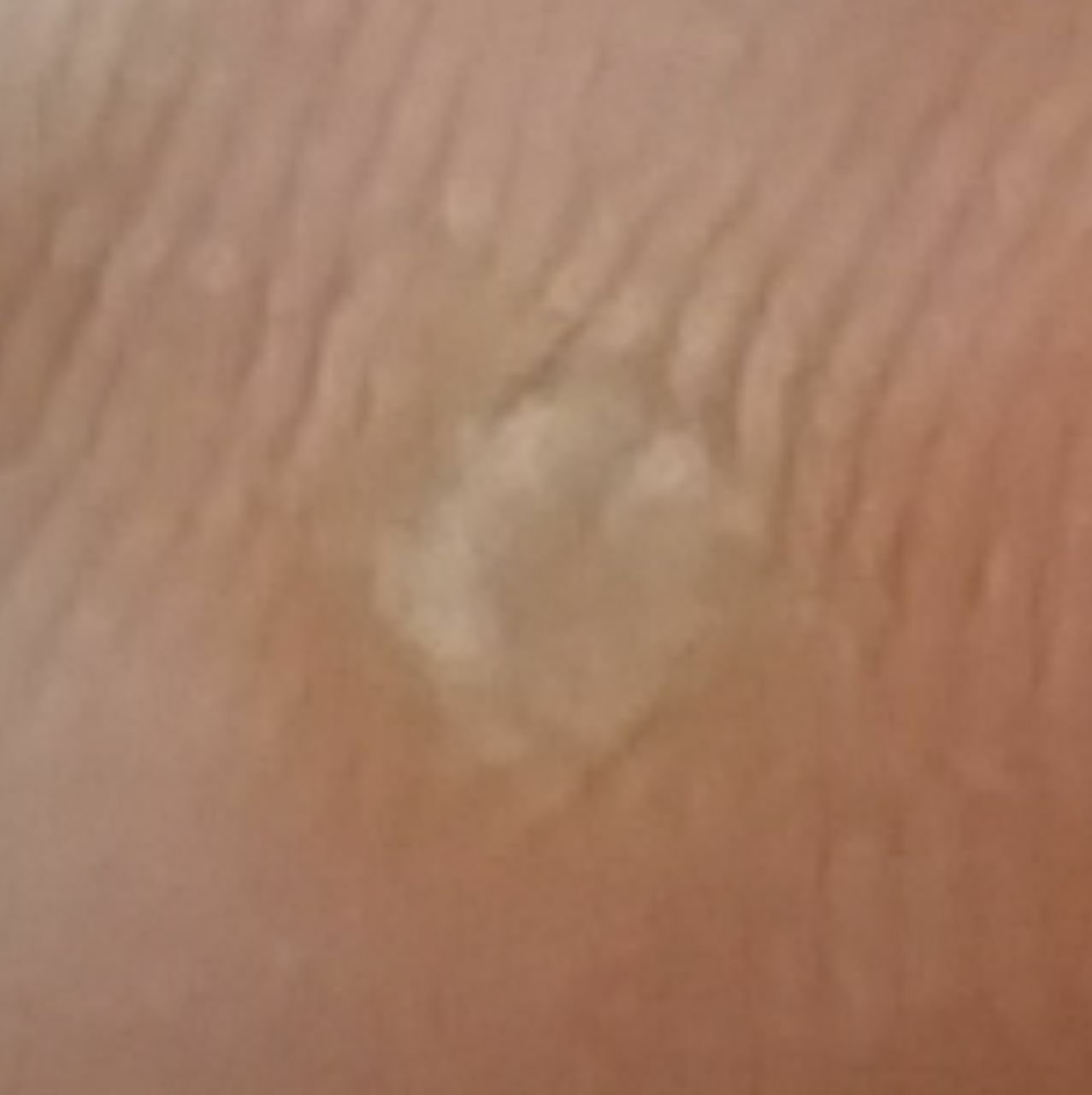
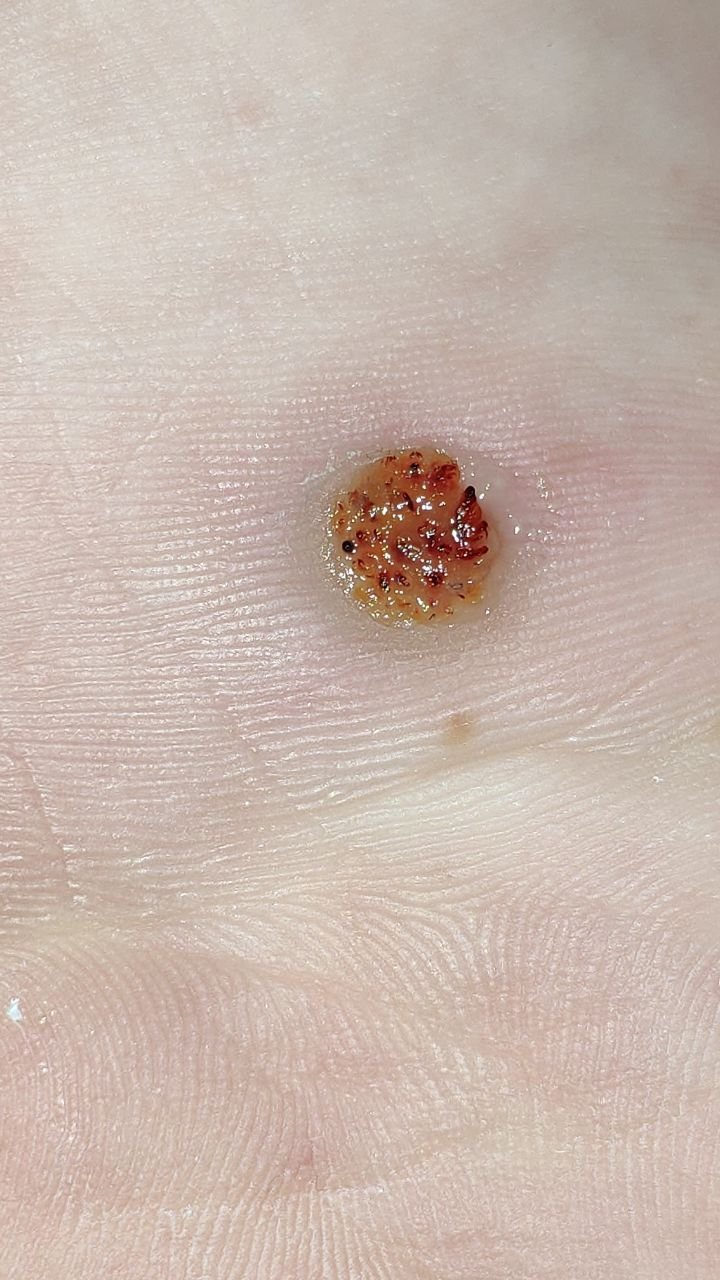
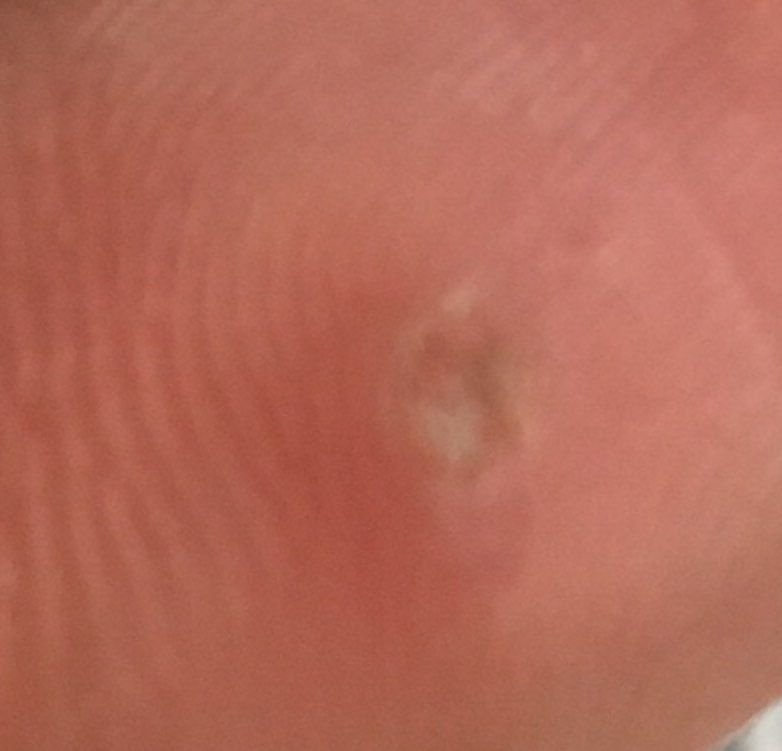
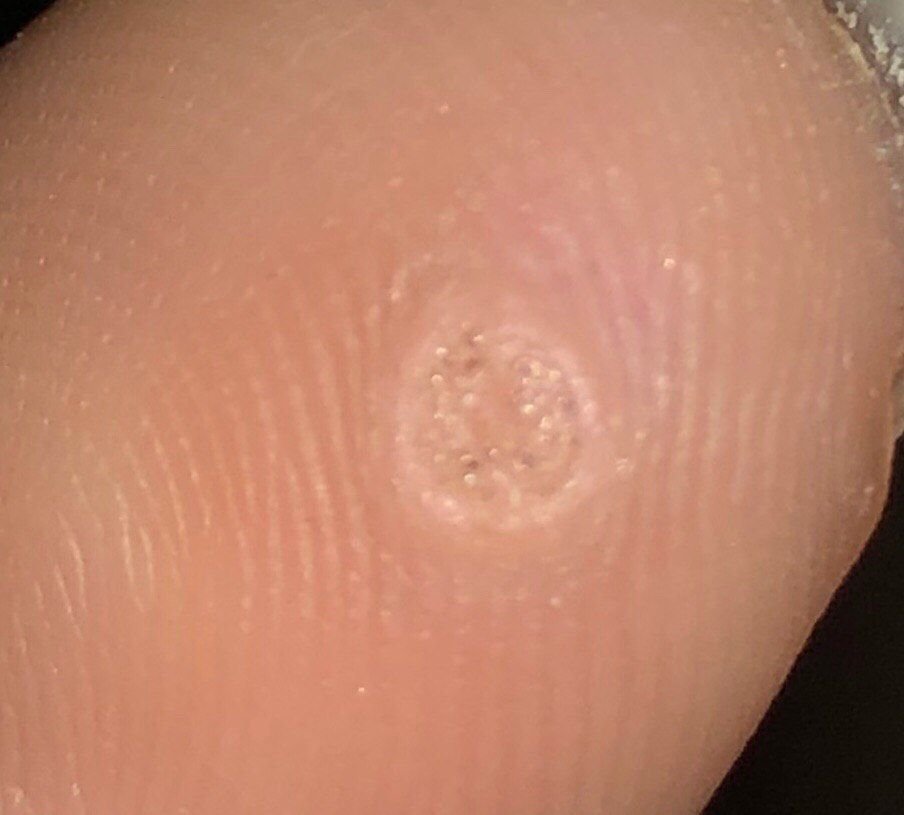
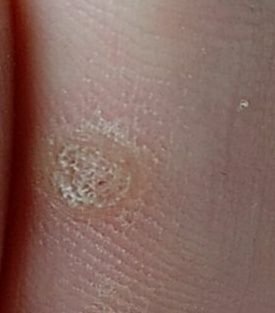
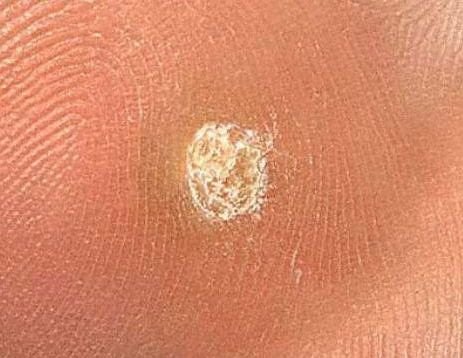
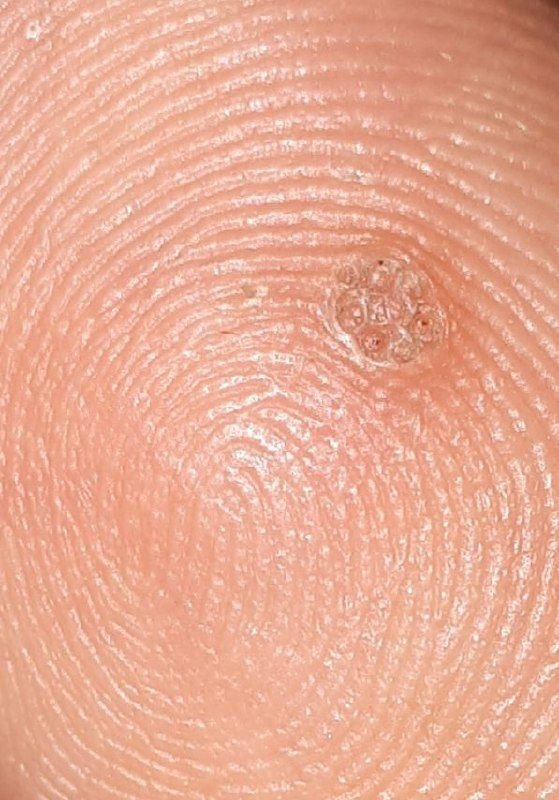
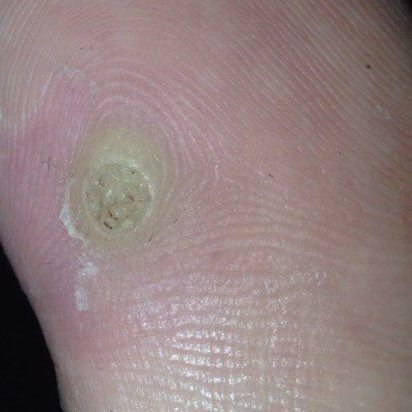
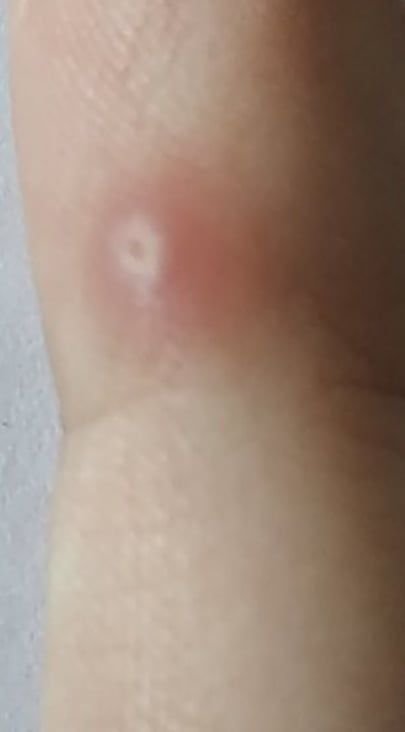
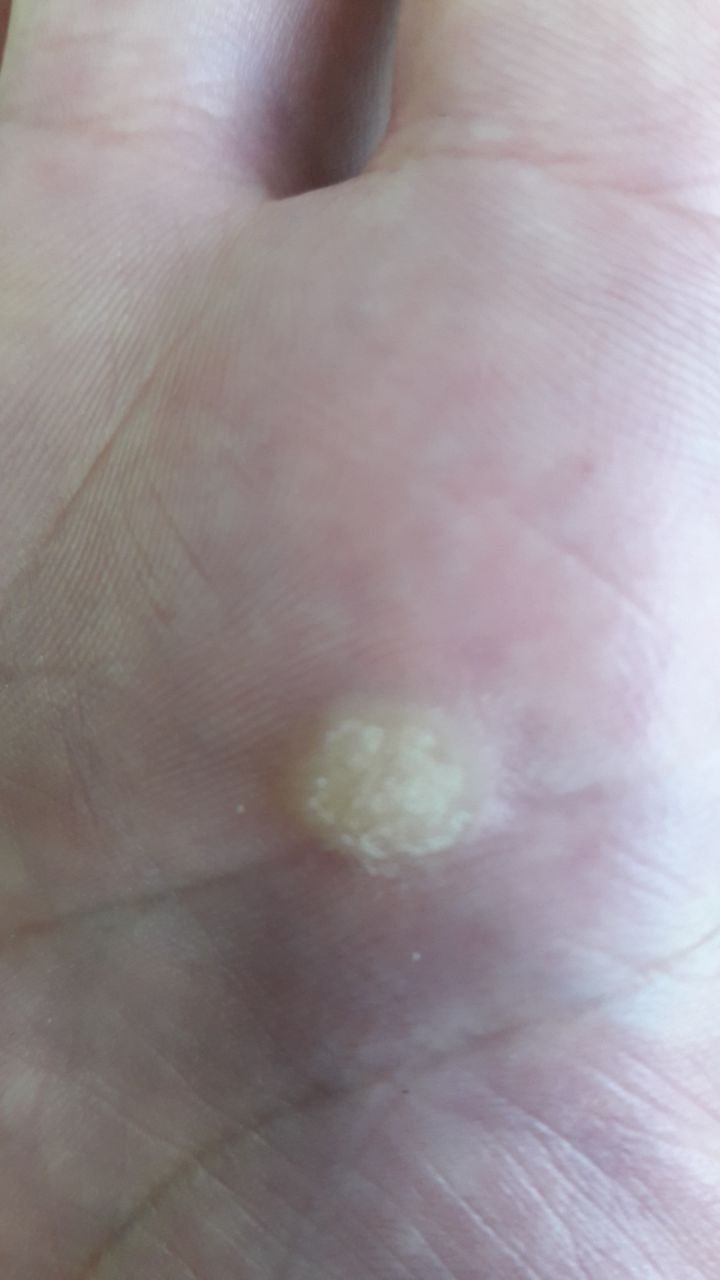
Common warts appear as small, skin-colored or slightly grayish papules with a rough, irregular surface. Their papillomatous architecture resembles miniature cauliflower-like growths. They may be solitary or grouped, and in some cases, lesions coalesce to form conglomerates.
Key clinical features include:
- Location: Predominantly found on the hands, fingers, and periungual areas; occasionally on the face, knees, or body;
- Size: Typically 2–5 mm in diameter and 1–3 mm in elevation; larger or confluent lesions may exceed 1 cm;
- Surface texture: Keratinized, dry, and rough to touch with tiny projections;
- Color: Usually flesh-toned or pale gray; keratin buildup may give a darker appearance;
- Edges: Clearly demarcated with a “cliff-like” corolla from adjacent healthy skin;
- Hair growth: Absent on the wart surface, but surrounding skin may have normal follicles;
- Symptoms: Typically asymptomatic, but pressure may cause tingling or discomfort—especially in palmar or plantar warts.
Dermatoscopic Description
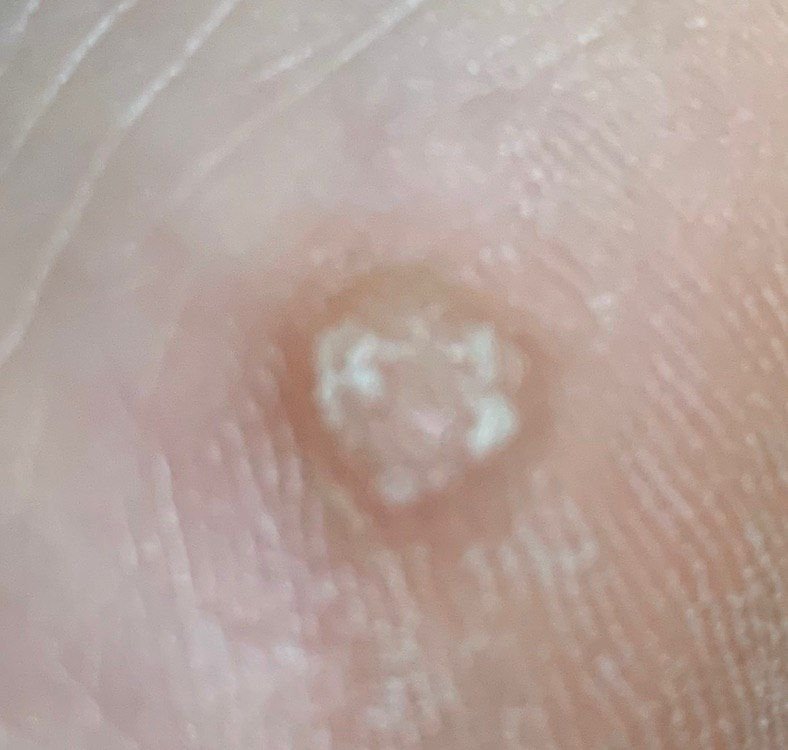
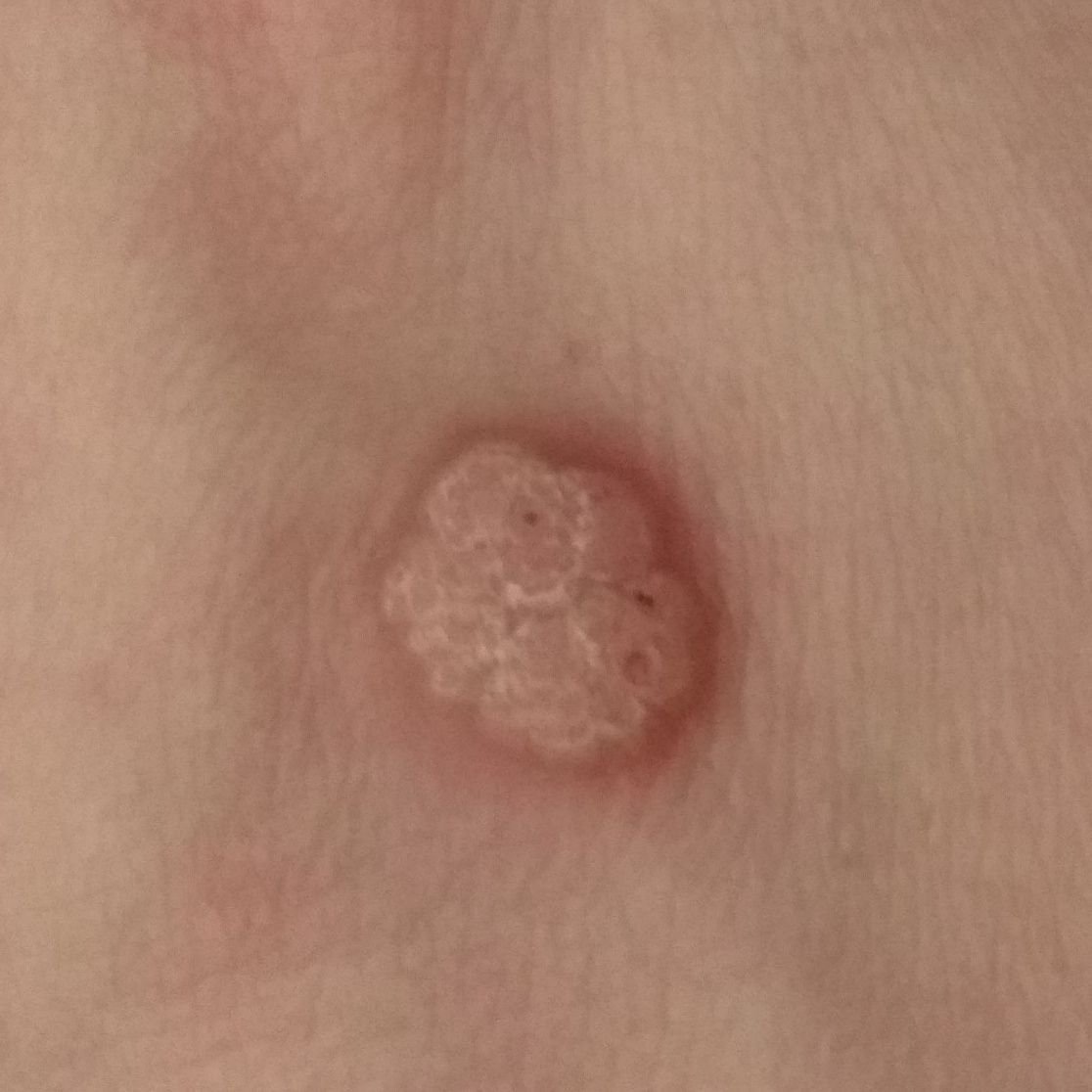
Dermatoscopy offers non-invasive visualization of key features that aid in confirming the diagnosis of viral warts. Hallmark dermatoscopic patterns include:
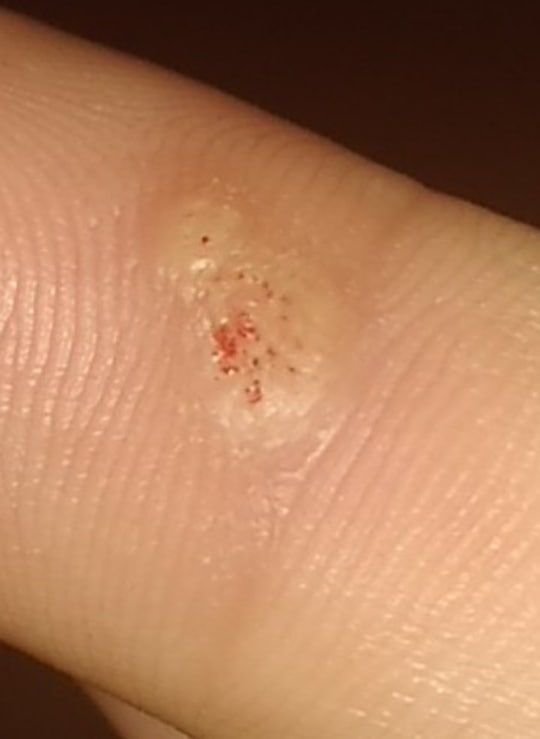
- “Frogspawn” appearance: Densely packed, keratinized papillae with a central red dot (feeding capillary);
- Thrombosed capillaries: Seen as black or brown dots within the lesion, representing clotted vessels;
- Pale corolla: A halo of keratin around the lesion marking a clear boundary with healthy skin;
- Lack of pigment network: Differentiates viral warts from pigmented nevi or melanomas.
These dermatoscopic features are crucial in distinguishing verruca vulgaris from other skin lesions such as seborrheic keratoses, melanocytic nevi, and malignancies.
Differential Diagnosis
Although the diagnosis of common warts is often straightforward, a number of other dermatological conditions can present with similar morphology. Accurate differentiation is important, particularly for persistent or atypical lesions. The differential diagnosis includes:
- Papillomatous nevus: Typically more pigmented, with longer-term presence and possible congenital history;
- Nevus sebaceous: Yellowish, plaque-like lesions usually seen on the scalp or face from early childhood;
- Halo nevus: Pigmented mole surrounded by a depigmented halo—no keratinization;
- Dermatofibroma: Firm nodules with a “dimple sign” when pinched;
- Flat wart (verruca plana): Smoother, smaller, and more often seen in young people on the face or extremities;
- Plantar wart: Located on the soles of the feet, often painful and embedded in skin creases;
- Molluscum contagiosum: Dome-shaped lesions with central umbilication and soft, white core;
- Basal cell carcinoma (nodular form): Pearly, slow-growing nodule, may ulcerate or bleed;
- Amelanotic melanoma: Rare, rapidly evolving lesion that lacks pigmentation—biopsy required for confirmation.
Risks: Clinical Significance of Warts
From an oncological standpoint, common warts are considered benign and do not pose a significant risk of malignancy. However, vigilance is required in lesions that exhibit suspicious features, such as:
- Sudden and rapid growth;
- Increased firmness or change in consistency;
- Ulceration, bleeding, or spontaneous pain;
- Color changes or irregular borders.
Besides cosmetic discomfort, warts may cause functional and hygiene issues:
- Trauma: Warts on hands are prone to repeated irritation and injury, leading to bleeding and risk of secondary infection;
- Autoinoculation: Scratching or damaging one wart can lead to multiple new lesions on adjacent skin;
- HPV carriage: Even asymptomatic carriers can transmit low-risk HPV to others or to other parts of their body.
Tactics: Clinical Strategy and Monitoring
For warts that remain unchanged and do not cause symptoms or trauma, simple observation with annual self-checks may be sufficient. However, dermatologic evaluation is advised when:
- There is mechanical injury, friction from clothing or jewelry;
- The wart changes in appearance or sensation (e.g., becomes painful, bleeds);
- There is significant cosmetic or psychological impact;
- The patient belongs to a high-risk group (e.g., immunocompromised, multiple neoplasms);
- The wart is located in high-friction or occupationally sensitive areas.
During monitoring, dermatologists often use photographic documentation and compile a skin lesion map to detect subtle changes over time.
Treatment of Common Warts
Removal is indicated when warts are symptomatic, rapidly growing, cosmetically disturbing, or at risk of frequent trauma. Preferred minimally invasive methods include:
- Laser ablation: Precise and effective for resistant or cosmetically sensitive areas;
- Cryotherapy: Application of liquid nitrogen to freeze the lesion; may require multiple sessions;
- Radiofrequency excision: Controlled destruction of tissue using high-frequency energy;
- Electrocoagulation: Thermal removal using electrical current under local anesthesia;
- Surgical excision with histology: Reserved for atypical lesions or where malignancy is suspected.
Self-removal is not recommended due to risks of bleeding, infection, and viral spread. Any treatment must be conducted under sterile conditions by trained professionals.
Prevention of Common Warts
Preventive strategies focus on reducing HPV exposure, supporting immune function, and maintaining skin integrity. Key recommendations include:
- Maintain personal hygiene: Avoid sharing personal items, especially in communal environments like gyms or swimming pools;
- Boost immune health: Proper nutrition, stress reduction, and management of chronic diseases help reduce HPV reactivation risk;
- Protect skin from trauma: Use gloves, avoid overexposure to UV and ionizing radiation, and minimize chronic irritation;
- Limit direct contact: Avoid touching known warts (yours or others) and wash hands frequently;
- Regular skin checks: Especially for individuals with a history of viral warts or other skin neoplasms;
- HPV vaccination: Although designed to prevent oncogenic strains, the vaccine may offer indirect protection against some cutaneous HPV types.
With early diagnosis, proper management, and responsible self-care, most cases of verruca vulgaris can be effectively controlled—and the chances of recurrence or complications minimized.