Herpes Simplex (ICD-10: B00) ⚠️
Herpes Simplex Virus (HSV-1 and HSV-2): Clinical Overview and Management
General Characteristics
Herpes simplex is a widespread viral infection caused by DNA-containing herpes simplex viruses (HSV), classified in the ICD-10 under codes B00 (Herpesviral infections) and A60 (Anogenital herpesviral infection). These viruses have the ability to establish latency in the human nervous system after initial infection and may reactivate periodically under favorable conditions. Reactivation episodes often coincide with physiological or environmental triggers such as hypothermia, respiratory illnesses, skin trauma, hormonal fluctuations (e.g., menstruation), gastrointestinal dysfunction, mental stress, or immunosuppression.
Once the virus enters the body, it replicates locally in the epithelial tissue of the skin or mucous membranes. It then travels retrograde via sensory neurons to the dorsal root or trigeminal ganglia, where it becomes latent. The virus can persist in this dormant state indefinitely, reactivating spontaneously or in response to external stressors to cause recurrent lesions in the original site of infection.
Etiology: HSV-1 and HSV-2
There are two distinct types of herpes simplex virus:
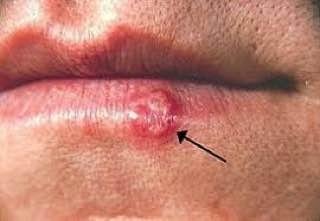
- HSV-1 (Herpes Simplex Virus Type 1): Primarily associated with oral and facial infections, particularly labial herpes, but can also cause genital infections through oral-genital contact.
- HSV-2 (Herpes Simplex Virus Type 2): Most commonly responsible for genital herpes, but can also infect the orofacial area in certain cases.
Both HSV-1 and HSV-2 are highly contagious and capable of causing acute symptomatic outbreaks as well as asymptomatic viral shedding, which contributes significantly to the spread of infection. Importantly, both virus types can result in primary and recurrent disease in either the oral or genital region, depending on the mode of transmission.
Clinical Manifestations
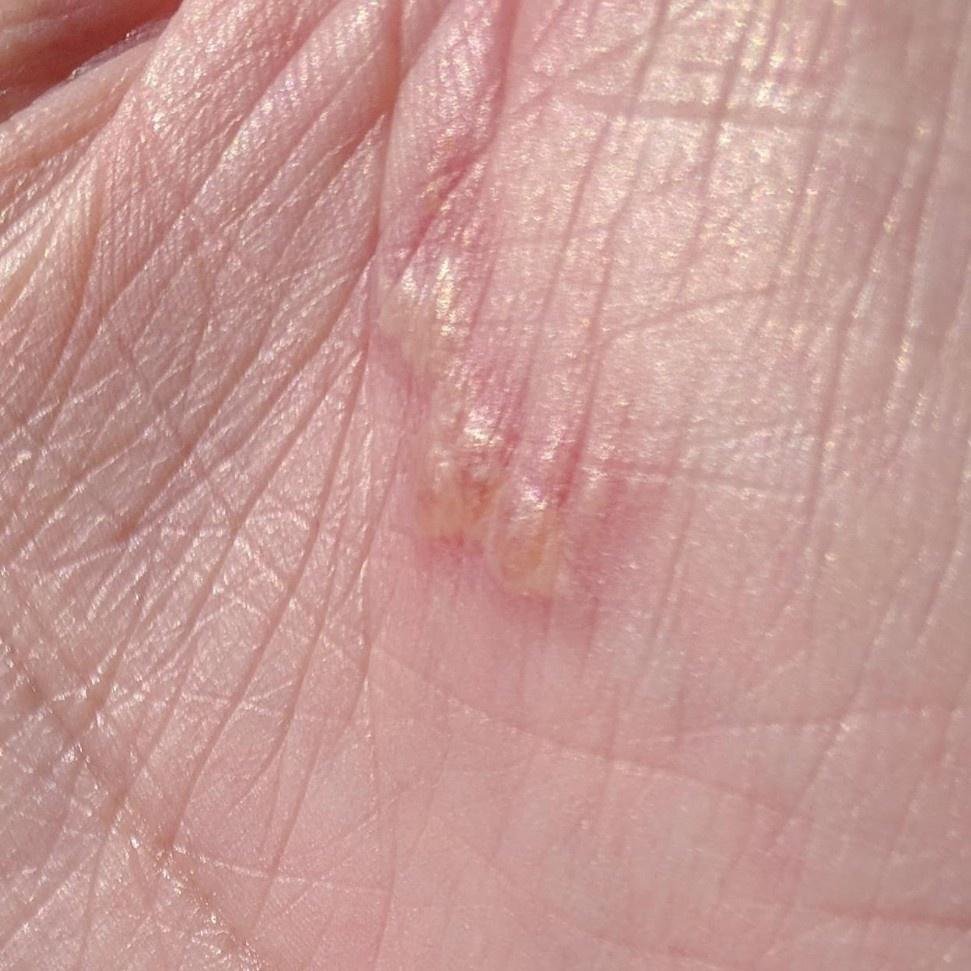
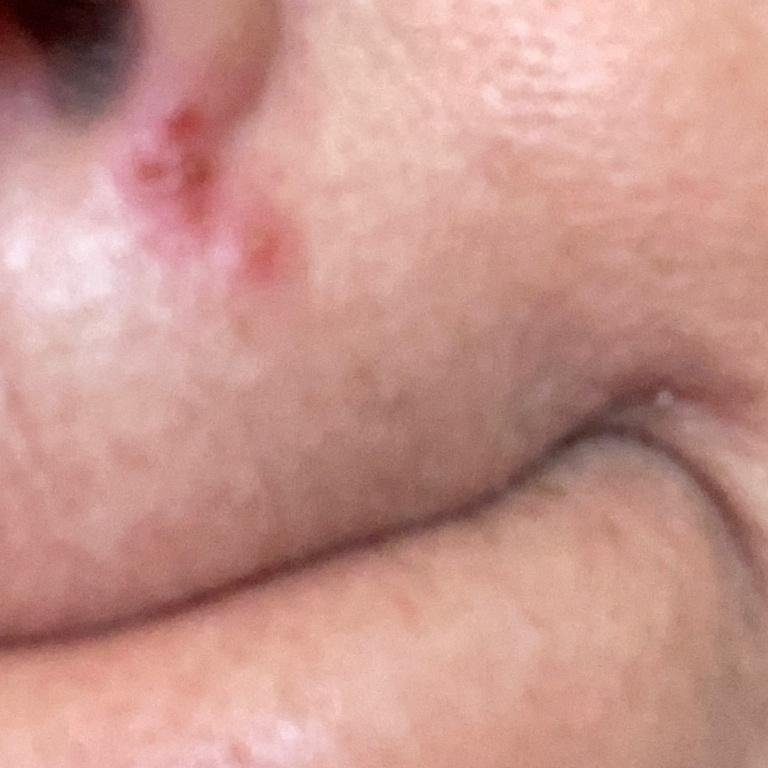
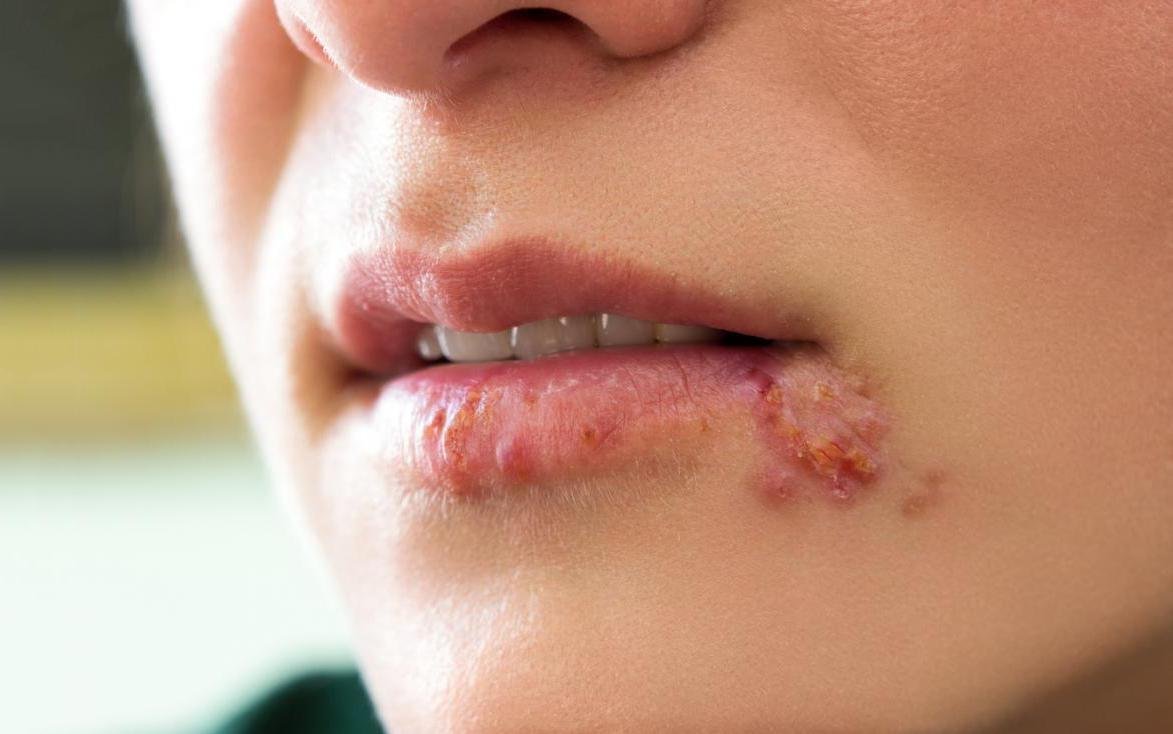
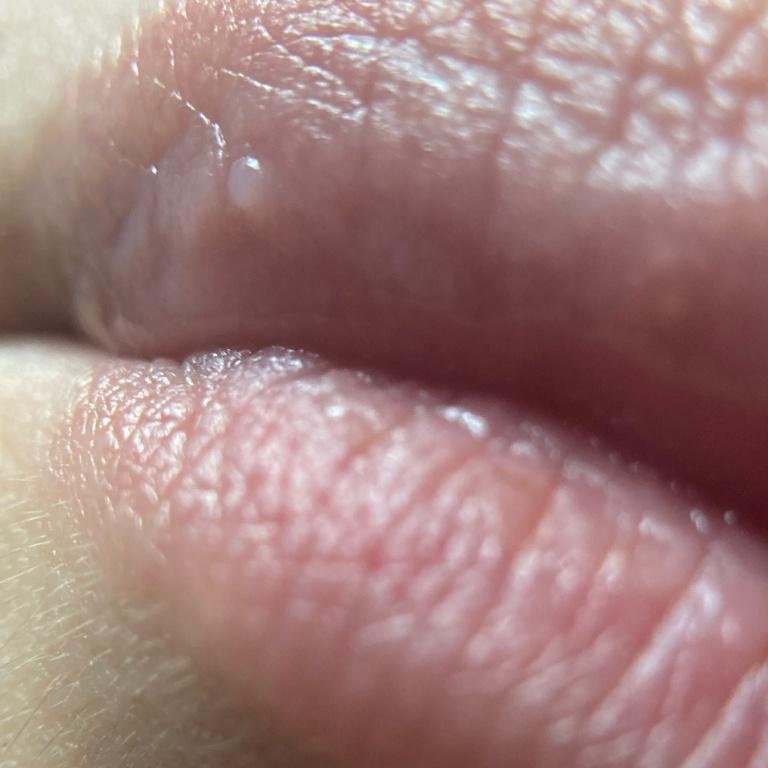
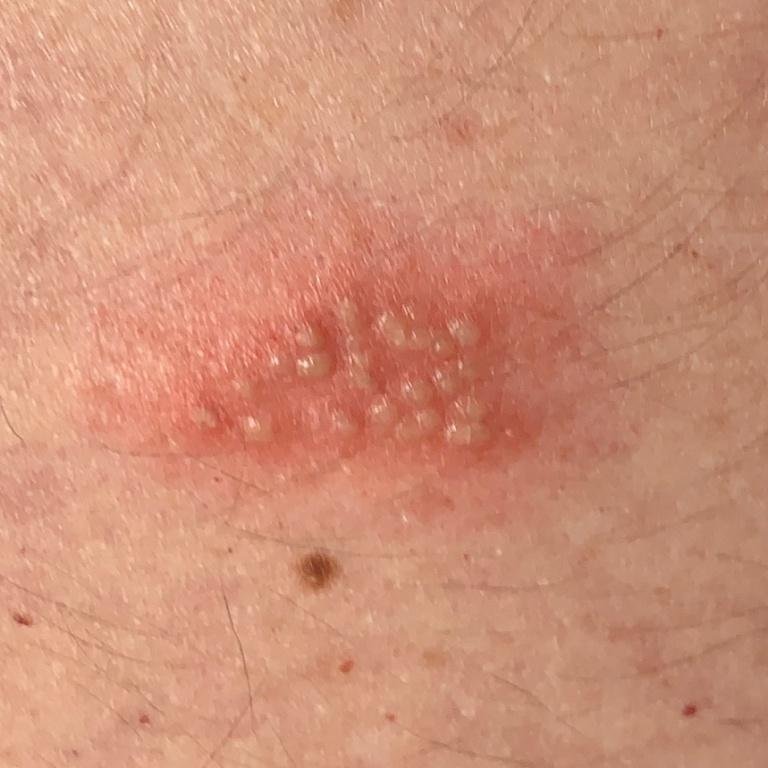
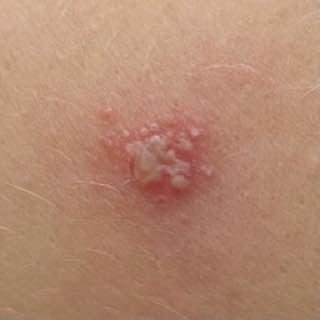
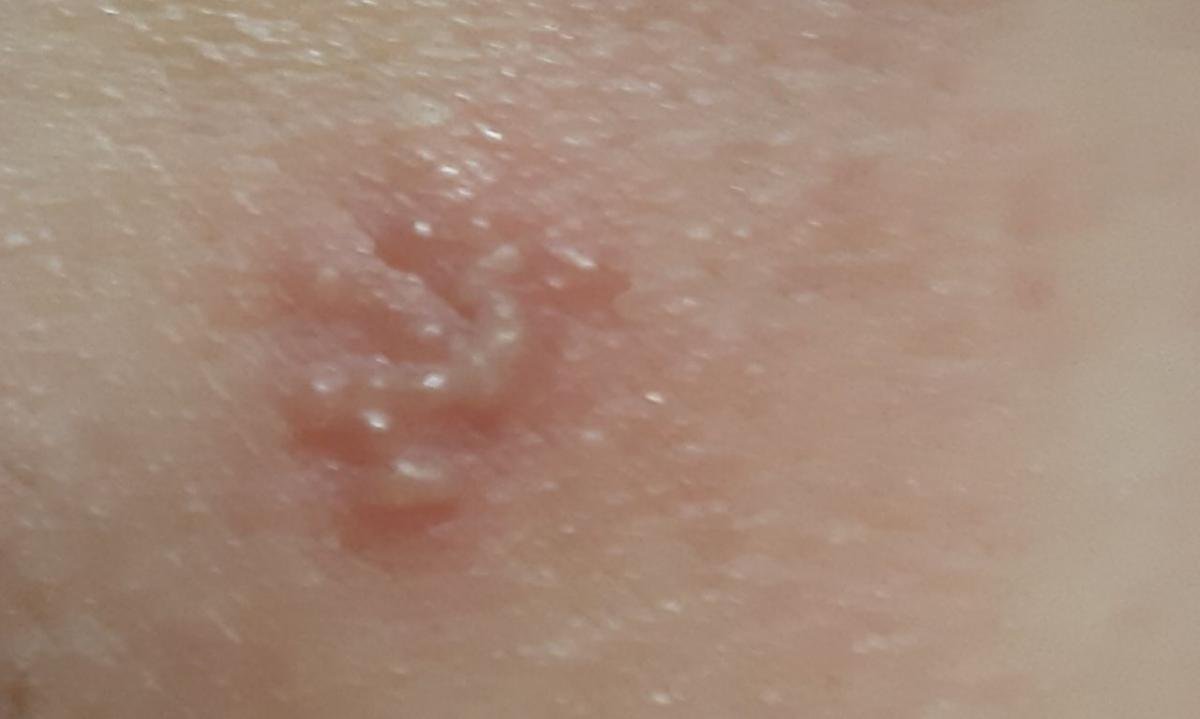
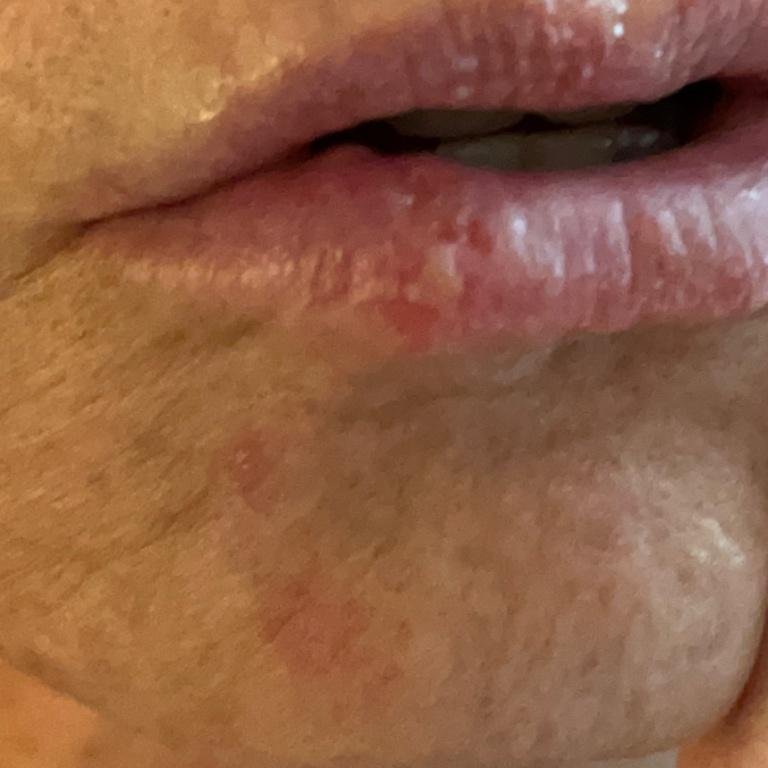
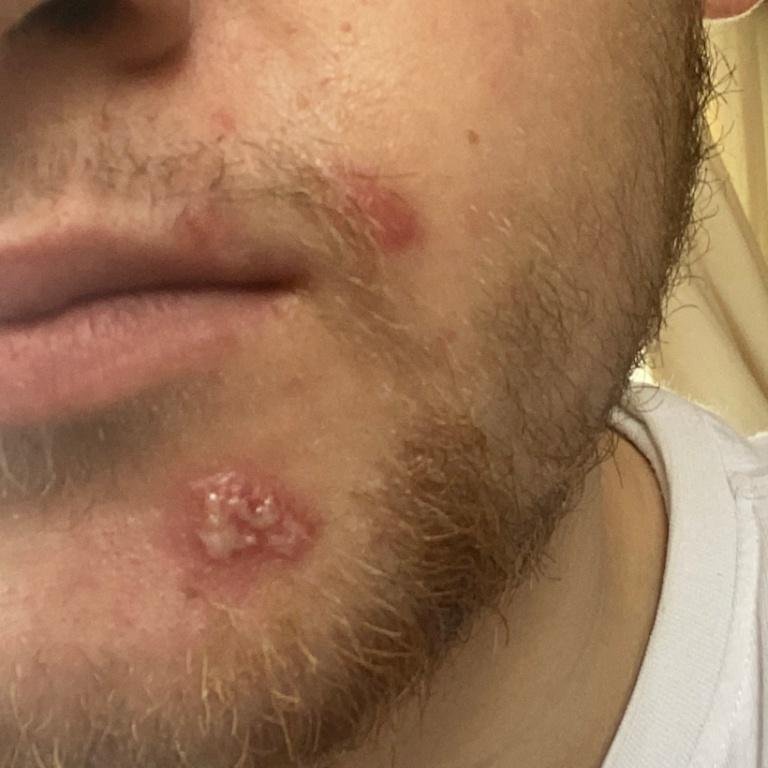
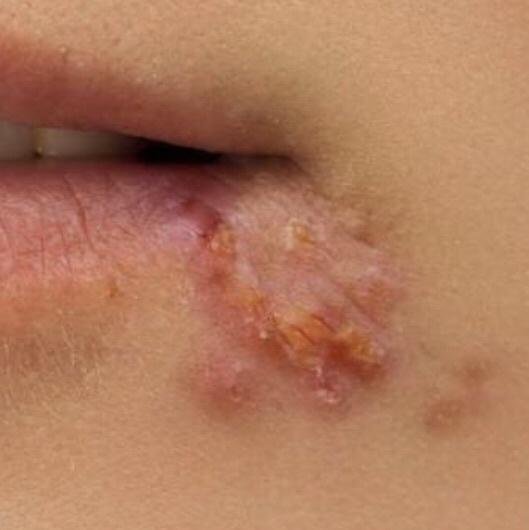
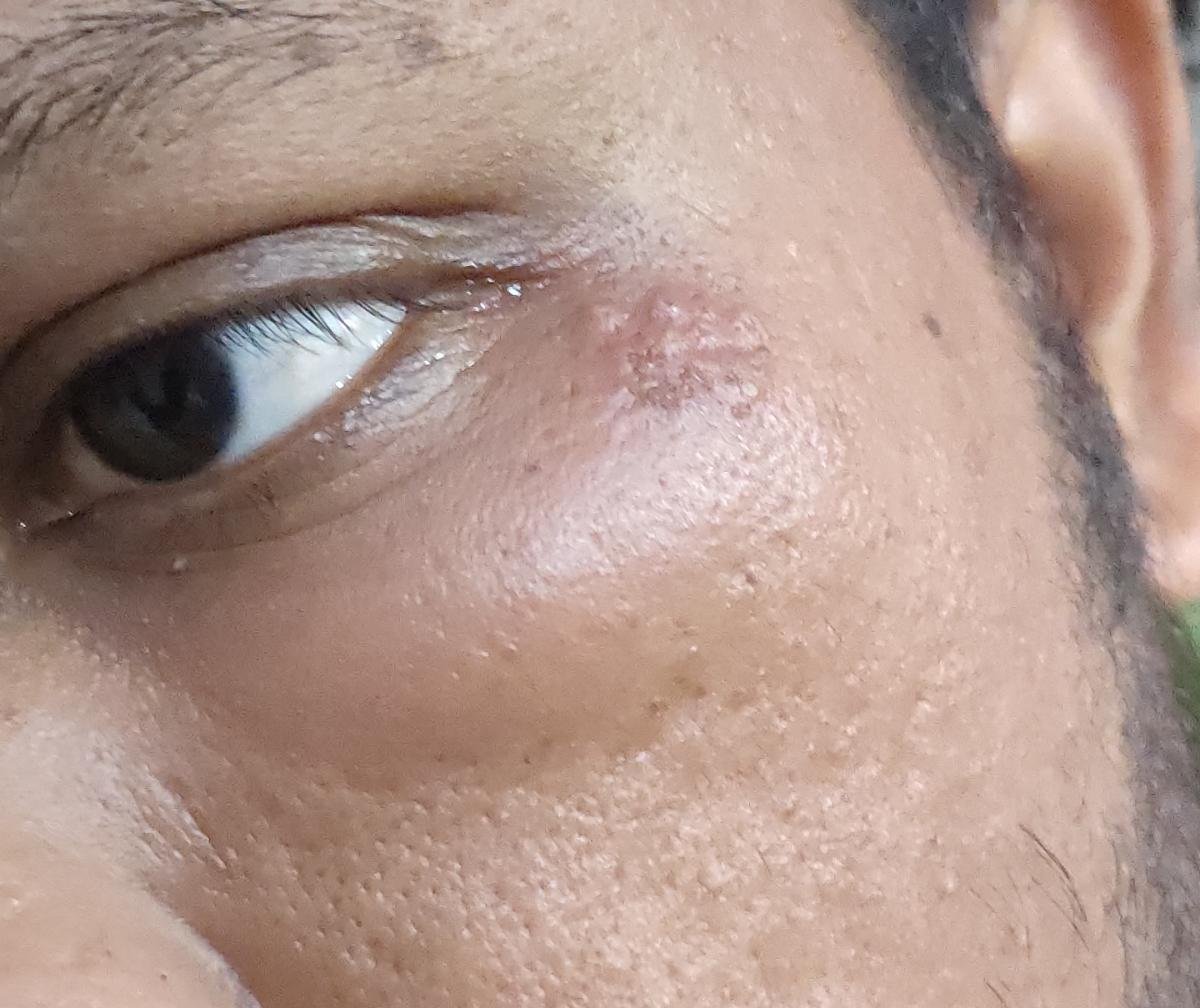
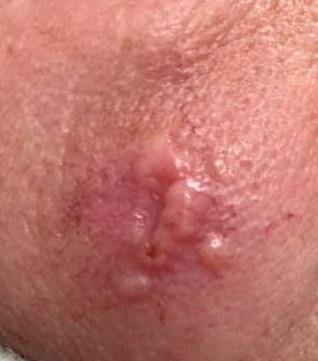
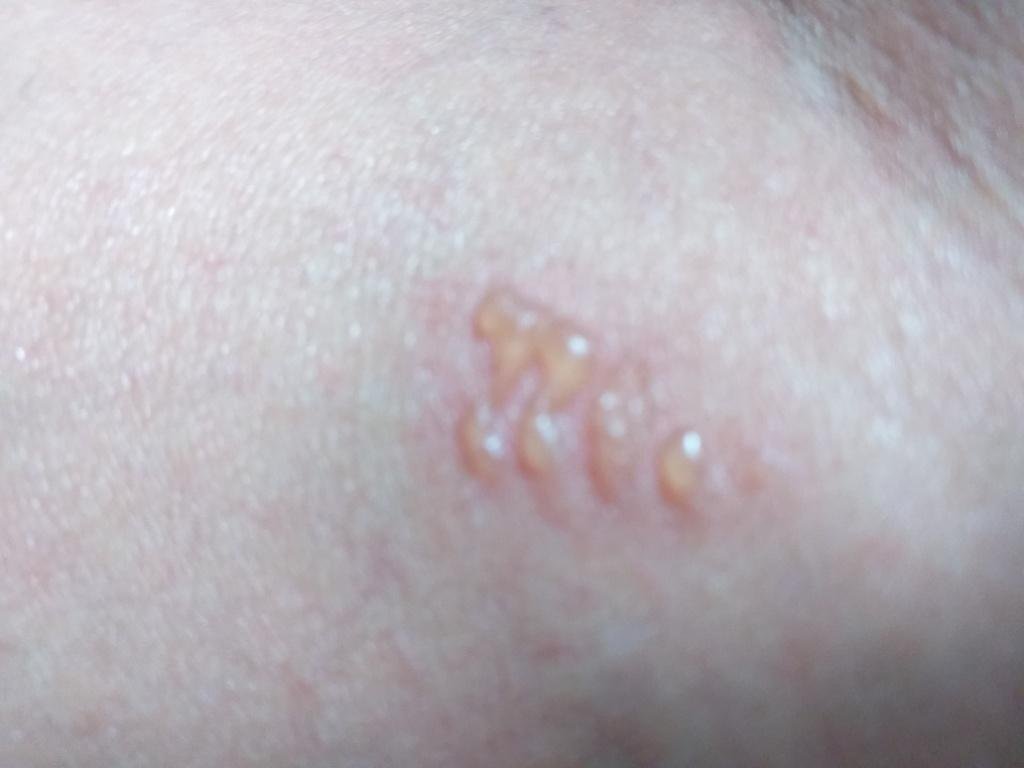
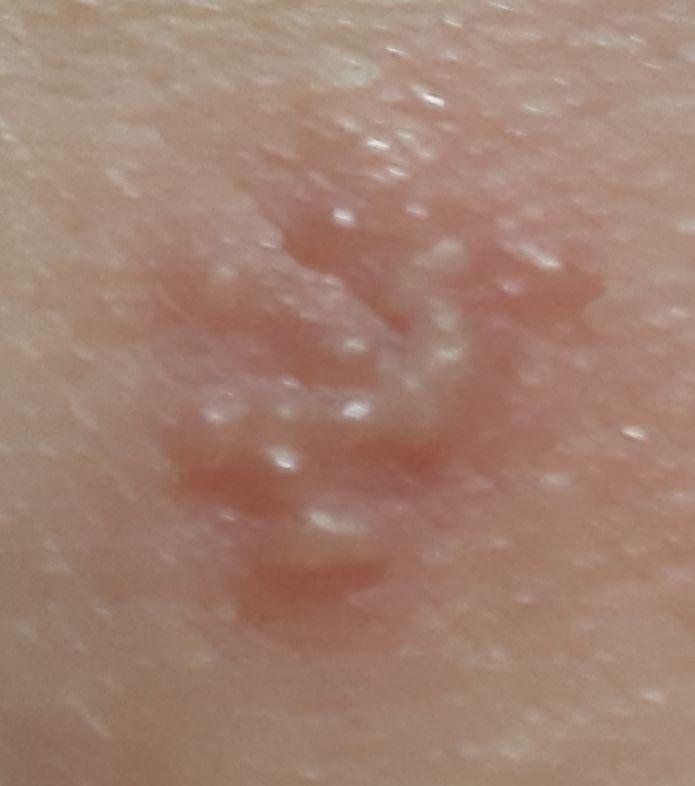
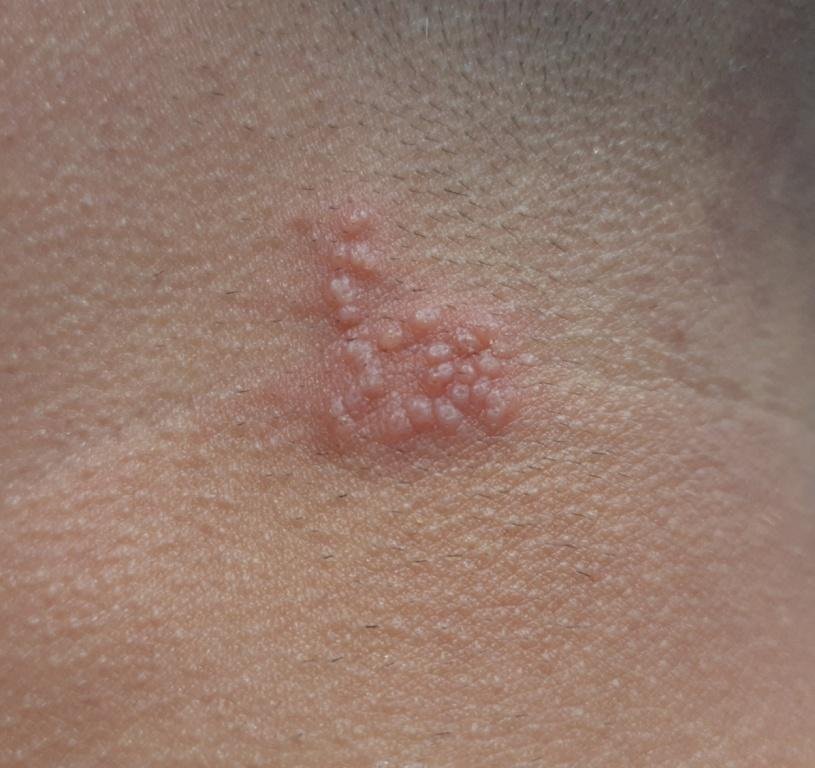
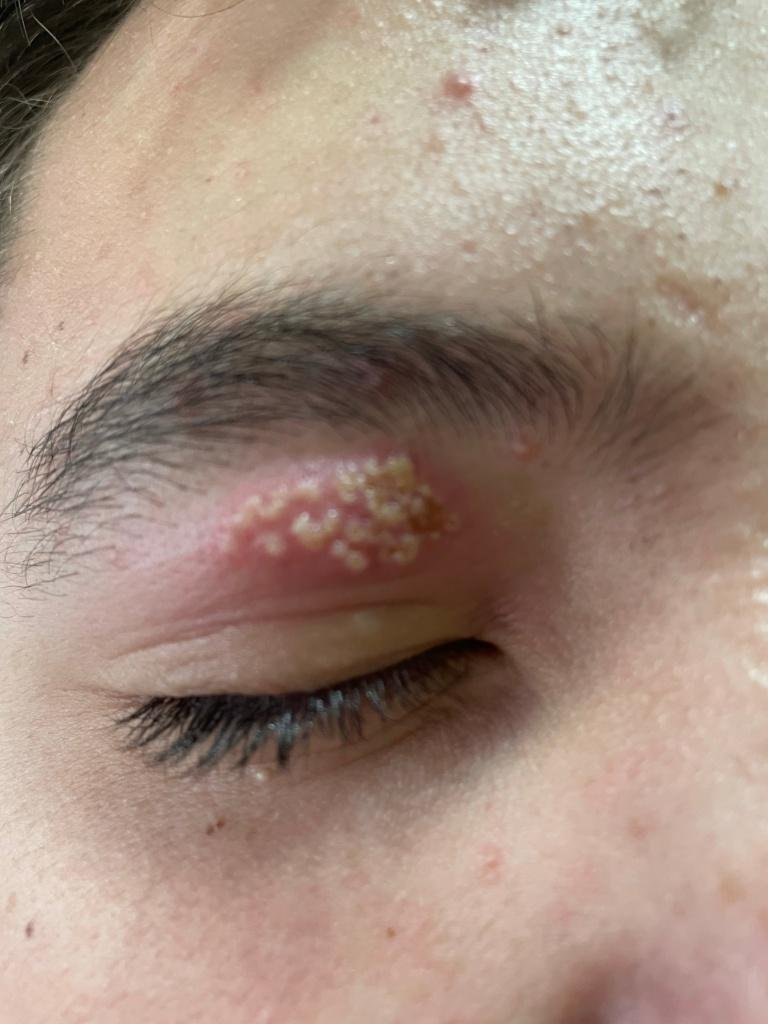
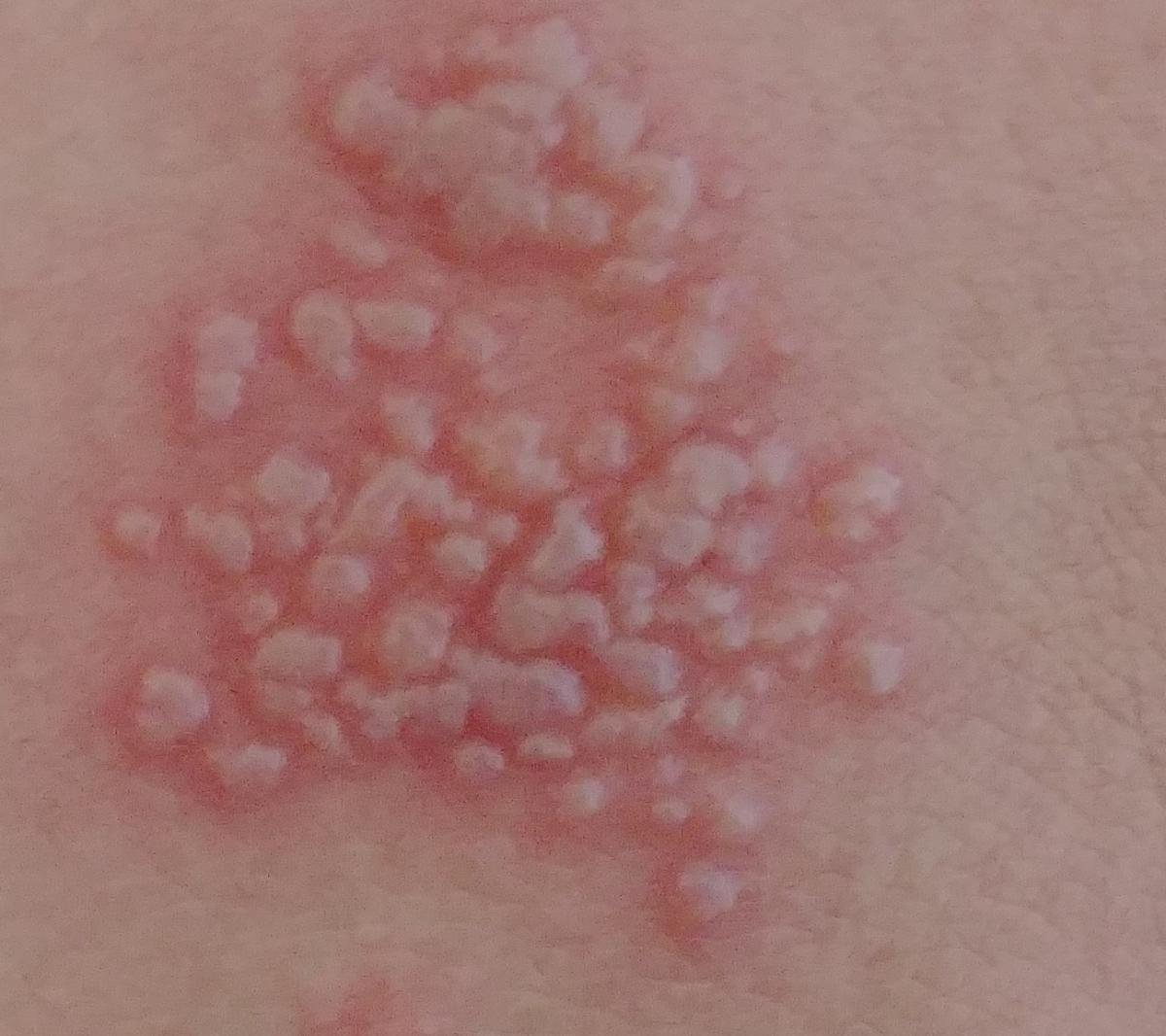
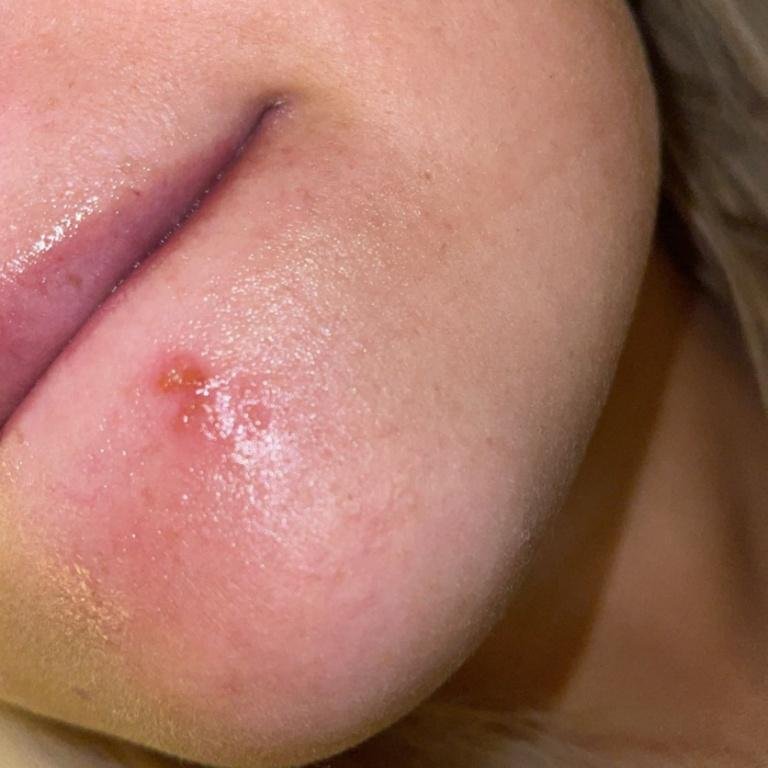
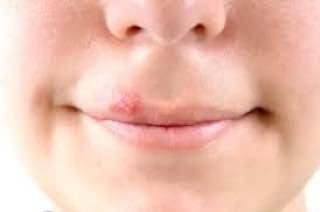
Herpes simplex infection typically presents as clusters of small, fluid-filled blisters (vesicles) on a red, swollen base. The vesicles are dome-shaped, ranging in size from 1–3 mm, and often coalesce into groups. Within 1 to 3 days, the fluid inside the vesicles becomes cloudy, and some may turn purulent or hemorrhagic. Eventually, the lesions rupture, leaving behind shallow ulcers that crust over and heal within 7–14 days.
Common locations include:
- HSV-1: Perioral region (lips, nose, cheeks), gingiva, palate, tongue, or facial skin;
- HSV-2: Genital and perineal region, buttocks, thighs, urethra, cervix, and vagina.
Subjective symptoms may include:
- Itching, tingling, or burning prior to the appearance of lesions (prodrome);
- Localized pain or discomfort in affected areas;
- Fever, fatigue, headache, and lymphadenopathy (especially in primary infections);
- Neuralgic pain: Especially common in genital herpes, often affecting the perineum, glans penis, or labia.
New blisters tend to appear in close proximity to initial lesions and may evolve over several days. Recurrent infections are usually milder and shorter in duration than the primary episode.
Diagnosis of Herpes Simplex Virus Infections
Although diagnosis is often based on the characteristic appearance of lesions and patient history, laboratory confirmation is essential in atypical cases, immunocompromised individuals, or when differentiating herpes from other ulcerative genital or oral conditions.
Recommended diagnostic methods include:
- Viral culture: Cultivation of HSV from fresh vesicular fluid; highly specific but less sensitive in recurrent episodes.
- Polymerase Chain Reaction (PCR): The most sensitive method, used to detect and type HSV DNA from lesion swabs, cerebrospinal fluid, or blood samples.
- Direct Fluorescent Antibody (DFA) Testing: Identifies viral antigens in lesion material; provides rapid results.
- Enzyme-Linked Immunosorbent Assay (ELISA): Serologic testing to detect type-specific HSV-1 and HSV-2 IgG antibodies, helpful for identifying prior exposure.
In cases of genital ulceration, differential diagnosis must include syphilis, chancroid, aphthous ulcers, and Behçet’s syndrome, among others. Therefore, combined clinical and laboratory approaches are the gold standard for accurate diagnosis.
Treatment of Herpes Simplex
While there is no cure for HSV infection, effective antiviral medications can significantly reduce the severity, duration, and recurrence rate of outbreaks. The choice of drug and dosing regimen depends on whether the infection is primary, recurrent, or prophylactic (suppressive).
Antiviral Medications:
- Acyclovir: The most widely used antiviral, available in oral, topical, and intravenous forms;
- Valacyclovir: A prodrug of acyclovir with better oral bioavailability, allowing for less frequent dosing;
- Famciclovir: An alternative with similar efficacy and good absorption characteristics.
Therapeutic approaches:
- Acute treatment: 5–10 day course initiated at the first sign of symptoms to reduce outbreak duration and transmission risk;
- Suppressive therapy: Daily antiviral use in patients with frequent recurrences or in discordant couples to minimize transmission;
- Topical formulations: May be used for localized relief, though systemic therapy is more effective overall.
In severe or complicated HSV infections (e.g., encephalitis, neonatal herpes, or disseminated disease), hospitalization and intravenous antiviral therapy may be required.
Prevention of Herpes Simplex Virus Infections
Preventing HSV transmission relies on a combination of behavioral precautions, barrier protection, partner communication, and immune system support. While complete prevention of herpes simplex transmission may not always be possible, the following strategies significantly reduce the risk of infection or reactivation:
Primary Prevention: Avoiding Initial Infection
- Consistent use of condoms: While not 100% protective, condoms reduce the risk of transmission by limiting skin-to-skin contact with infected areas.
- Avoiding sexual contact during active outbreaks: HSV shedding is highest when lesions are present; abstinence during flare-ups is essential.
- Partner disclosure: Inform sexual partners of known HSV infection and discuss testing for both HSV-1 and HSV-2.
- Post-exposure hygiene: Thorough washing of hands and genitals after sexual activity can help reduce viral contact risk.
- Screening and testing: Individuals with multiple partners or in new relationships should consider STI panels that include HSV-specific serology.
Secondary Prevention: Reducing Recurrence and Transmission
For individuals already infected with HSV, the goal is to minimize outbreaks and reduce the chance of spreading the virus to others. Recommendations include:
- Daily antiviral prophylaxis: For patients with frequent recurrences or in serodiscordant couples, suppressive therapy with acyclovir, valacyclovir, or famciclovir is highly effective in reducing outbreaks and asymptomatic shedding.
- Identifying and avoiding personal triggers: Maintain a journal to track the onset of symptoms and correlate with stress, illness, or lifestyle changes.
- Immune system support: Balanced nutrition, adequate rest, stress reduction techniques, and treatment of chronic illnesses help reduce reactivation risk.
- Avoiding skin trauma: Friction during intercourse, shaving, or abrasive clothing may trigger outbreaks, especially in the genital region.
Conclusion
Herpes simplex virus (both HSV-1 and HSV-2) is a pervasive and lifelong infection with significant implications for physical and emotional well-being. Despite the absence of a definitive cure, modern antiviral treatments provide reliable control over symptoms, reduce transmission risk, and allow most individuals to lead normal, fulfilling lives.
Through early diagnosis, education, preventive strategies, and tailored therapeutic regimens, both primary and recurrent HSV infections can be effectively managed. Public awareness and responsible sexual behavior remain critical components in reducing the global burden of herpes simplex infections.
Individuals who suspect HSV infection—or are managing known herpes—should work closely with healthcare providers to establish personalized care plans and maintain optimal skin and sexual health.